Giving men with suspected prostate cancer an MRI scan could improve diagnosis and save those who do not have aggressive cancers from having an unnecessary biopsy, according to a study published in The Lancet.
The study estimates that adding the extra test could help one in four (27%) men avoid an unnecessary biopsy and reduce the number of men who are over-diagnosed – diagnosed with a cancer that does not go on to cause any harm during their lifetime – by 5%.
Typically, men undergo a biopsy of their prostate if they experience symptoms of prostate cancer or have a prostate specific antigen (PSA) test showing high levels of the PSA protein in their blood. Each year, over 100,000 prostate biopsies are carried out in the UK and one million are conducted in Europe. However, the PSA test is not always accurate, which means that many men undergo unnecessary biopsies.
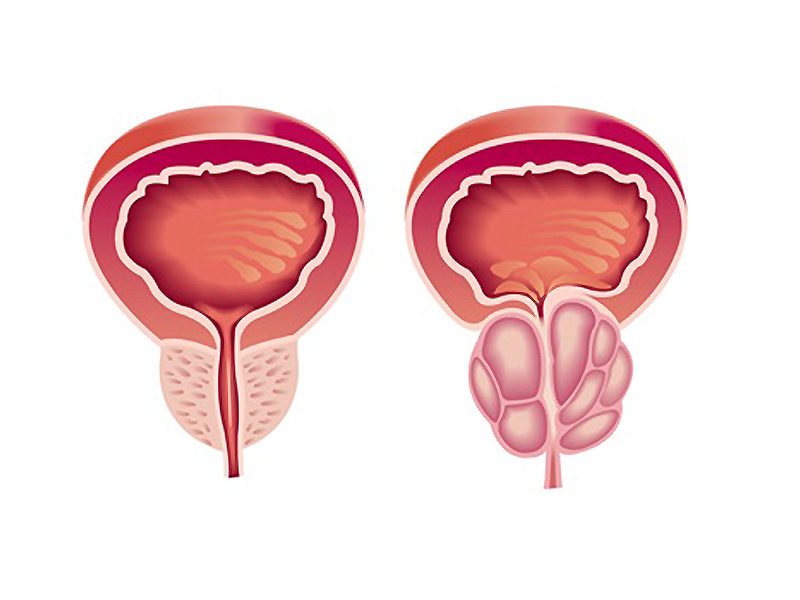
“Prostate cancer has aggressive and harmless forms. Our current biopsy test can be inaccurate because the tissue samples are taken at random. This means it cannot confirm whether a cancer is aggressive or not and can miss aggressive cancers that are actually there. Because of this some men with no cancer or harmless cancers are sometimes given the wrong diagnosis and are then treated even though this offers no survival benefit and can often cause side effects. On top of these errors in diagnosis, the current biopsy test can cause side effects such as bleeding, pain and serious infections.” said lead author, Dr Hashim Ahmed, UCL, UK. [1]
Multi-parametric MRI (MP-MRI) scans provide information about the cancer’s size, how densely packed its cells are and how well connected to the bloodstream it is, so could help differentiate between aggressive and harmless cancers.
In this study, 576 men with suspected prostate cancer were given an MP-MRI scan followed by two types of biopsy in 11 NHS hospitals. Firstly, they underwent a template prostate mapping (TPM) biopsy, which was used as a control to compare the accuracy of the MP-MRI and standard biopsy against. The second biopsy was the standard transrectal ultrasound-guided (TRUS) biopsy – the most commonly used biopsy for diagnosing prostate cancer.
The TPM biopsy found that less than half of the men in the study (40%) had aggressive cancer.
Of these, the MP-MRI scan correctly diagnosed almost all of the aggressive cancers (93%), whereas the TRUS biopsy correctly diagnosed only half (48%). Further, for men who had a negative MP-MRI scan, nine out of 10 (89%) had either no cancer or a harmless cancer.
Because of this, the researchers suggest that MP-MRI could be used before TRUS biopsy to identify those who have harmless cancers and do not need a biopsy immediately. This group could instead continue to be monitored by their doctors, while those thought to have aggressive cancers could then have their MP-MRI scan result confirmed by the TRUS biopsy. Overall, this would reduce over-diagnosis while improving detection of aggressive cancers.
“Our results show that MP-MRI should be used before biopsy. Our study found that using the two tests could reduce over-diagnosis of harmless cancers by 5%, prevent one in four men having an unnecessary biopsy, and improve the detection of aggressive cancers from 48% to 93%,” said Dr Hashim Ahmed. “While combining the two tests gives better results than biopsy alone, this is still not 100% accurate so it would be important that men would still be monitored after their MP-MRI scan. Biopsies will still be needed if an MP-MRI scan shows suspected cancer too, but the scan could help to guide the biopsy so that fewer and better biopsies are taken.” 1
During the study there were 44 serious adverse events, with eight cases of sepsis caused by a urinary tract infection and 58 cases of urinary retention. These were a result of the biopsies rather than the MP-MRI scan, and are symptoms commonly seen in the clinic as a result of the standard biopsy.
Limitations of the study include that giving the TPM biopsy before the TRUS biopsy may have caused swelling and changes to the prostate tissue which could affect the accuracy of the TRUS biopsy. In addition, more research is needed into the cost-effectiveness of this approach, how it affects hospital capacity and ensuring there are enough radiologists to conduct the MP-MRI in the NHS.
The study was funded by the UK Department of Health, National Institute for Health Research, The University College London Hospitals Biomedical Research Centre and the Royal Marsden and Institute of Cancer Research Biomedical Research Centre. It was conducted by scientists from UCL, UCLH NHS Foundation Trust, the Royal Marsden Hospital, the MRC Clinical Trials Unit at UCL, University of York and Hampshire Hospitals NHS Foundation Trust.
Article: Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study, Hashim U Ahmed, FRC et al., The Lancet, doi: 10.1016/S0140-6736(16)32401-1, published 19 January 2017.